The high costs of pain pill addiction
Not every opiate addict can afford the gold-standard treatment for pain pill addiction. Most addicted professionals and celebrities (and addicts lucky enough to get on Dr. Phil’s show) go to inpatient treatment centers where they undergo medically managed detoxification. This is followed by no less than one month of inpatient residential treatment, and when they leave the treatment facility, they continue treatment with outpatient counseling.
But what about opiate addicts who don’t have insurance to pay for effective inpatient treatment, or who have insurance, but can’t support their families if they go away to treatment for a month or so? What are their options?
Many opiate addicts cycle in and out of detox units, staying only five to seven days, because that’s all they can afford. This limited treatment produces relapse rates of at least ninety percent. Methadone maintenance programs, despite forty-five years of evidence that it works, still have such a stigma attached to the therapy that, unfortunately, many opiate addicts refuse to consider this option.
Buprenorphine is an innovative option.
Buprenorphine just a substitute?
Critics say that using buprenorphine is merely exchanging one drug for another, and they’re right, but there’s a reason for using it. The pharmacological principle behind buprenorphine is the same as with methadone: both are long-acting opiate medications, which when dosed properly, prevent opioid withdrawal for more than twenty-four hours (a much better option than cold turkey OxyContin withdrawal), and don’t cause a euphoric high. Instead of endless cycle of intoxication and withdrawal, addicts on a stable dose of buprenorphine feel normal. If they relapse while on buprenorphine, they won’t feel it, since it blocks the high.
Buprenorphine vs. methadone
Buprenorphine is only a partial opiate, and less potent than methadone. With a full opiate like methadone, the more you take, the more opiate effect you feel. But with buprenorphine, maximum effect occurs at doses around 24 to 32 milligrams. After that, there’s no additional opiate effect. Therefore, it’s a safer drug than methadone, but not strong enough for some addicts with high opiate tolerances.
Because it’s a partial opiate, it was hoped that this drug would be easier than methadone to taper off, but that’s not everyone’s experience. Some patients are able to taper down to 2 to 4 milligrams, but feel intolerable withdrawal when they try to taper further. Others taper easily, but have difficulty avoiding relapses.
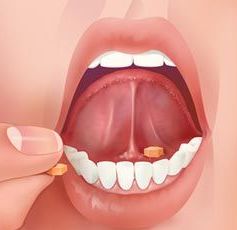
Buprenorphine sublingual tablets: what are they?
Buprenorphine may be better known by its manufacturer’s brand names, Suboxone and Subutex. Suboxone contains both buprenorphine and an anti-opiate called naloxone. Subutex contains only buprenorphine.
The naloxone in Suboxone is the generic name of Narcan, which is used by emergency medical personnel to reverse potentially fatal opiate overdoses. When the Suboxone tablet is used properly by dissolving under the tongue, no naloxone gets into the addict’s system. But if the addict dissolves the tablet in water and injects it, the Narcan is active, putting the addict into withdrawal. Therefore, Suboxone is felt to be a safer product, because it’s less likely to be abused by opiate addicts. Can Suboxone get you high?
Using buprenorphine correctly
The high cost of buprenorphine treatment and the relative scarcity of doctors authorized to prescribe it are the biggest obstacles to treatment with this drug. In most areas, office-based treatment with buprenorphine is more than twice the cost of treatment at a methadone clinic.
The medication isn’t meant to be used alone. Just like with methadone, medication is only one part of treatment. The best outcomes are seen with counseling and involvement with recovery groups.








Related Posts