A full guide to hydrocodone detox protocols here. ...


A full guide to hydrocodone detox protocols here. ...

Hydrocodone withdrawal does not need to be torture. Learn more about the medications and protocols used to address sympt ...

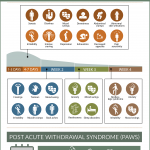
A visual guide to symptoms of hydrocodone withdrawal and the TIME OF THEIR APPEARANCE. What happens in the days and wee ...
An interview with practitioners of The Waismann Method® about how rapid opiate detox works, its safety, and what to exp ...

Practical suggestions for how to withdraw from hydrocodone safely. Plus. a section on How to ease withdrawal symptoms fr ...

What's the best way to withdraw from hydrocodone? Hydrocodone withdrawal treatment should ideally be individualized by ...

Going cold turkey off hydrocodone can be severe and is unnecessary. Learn more about cold turkey hydrcodone risks and be ...

Once you stop taking hydrocodone after regular use, a period of withdrawal will occur. Why? Because the brain compensate ...

Acute hydrocodone withdrawal occurs within the first few days after your last dose. Symptoms usually peak around 72 hour ...

Hydrocodone dependence can develop as quickly as three (3) weeks after regular dosing begins. More here about dependence ...

HOW OUR HELP LINE WORKS
For those seeking addiction treatment for themselves or a loved one, the Addictionblog.org helpline is a private and
convenient solution.
Calls to any general helpline (non-facility specific 1-8XX numbers) for your visit will be answered by
American Addiction Centers (AAC).
Caring admissions consultants are standing by 24/7 to discuss your treatment options. These representatives work
solely for AAC and will discuss whether an AAC facility may be an option for you.
Our helpline is offered at no cost to you and with no obligation to enter into treatment. Neither Addictionblog.org
nor AAC receives any commission or other fee that is dependent upon which treatment provider a visitor may
ultimately choose.
For more information on AAC’s commitment to ethical marketing and treatment practices, or to learn more about how to
select a treatment provider, visit our About AAC.
If you wish to explore additional treatment options or connect with a specific rehab center, you can browse top-rated listings, visit our homepage and browse by state, or visit SAMHSA.