SUMMARY: Morphine causes changes in the form and function of specific brain areas. It affects incentive motivation, reward, and learning. After a period of abstinence, some deficits can last for months or years after last use.
TABLE OF CONTENTS
- Main Brain Effects
- Define “Long Term”
- Nervous System
- Neurotransmitters
- Personality and Behavior
- Typical Dosing
- Occasional Tapering
Main Brain Effects
Prescription painkillers like morphine are used to treat moderate to severe pain and are often prescribed following surgery or injury, or for health conditions such as cancer. How does this strong painkiller work in the brain?

Morphine directly targets the central nervous system and changes the way in which the body feels and responds to pain. More precisely, it binds to opiate receptors in the brain to change the neurochemical activity in the brain stem which can result in alteration of the automatic body functions.
In recent years, there has been a dramatic increase in the acceptance and use of prescription opioids for the treatment of chronic, non-cancer pain, such as back pain or osteoarthritis, despite serious risks and the lack of evidence about their long-term effectiveness.
However, this strong painkiller also affects regions in the brain responsible for pleasure and with regular use the brain starts to register the effects of the morphine as a reward. According to the 2016 National Survey on Drug Use and Health (NSDUH):
- 6.8 million Americans used morphine in the past year.
- 536,000 people reported misuse of morphine in the past year.
So, if you’re worrying about long term use, you’re not the only one! How does morphine affect the brain, exactly? Keep reading to learn more.
Morphine can cause regional neuroplastic changes in the brain after only one month of daily administration.
How long is “long term”?
For short-term relief of severe acute pain morphine is used for about 4 weeks or 1 month. Long-term use is defined as using morphine for one month or longer, and is typically recommended for the management of severe chronic pain. However, morphine should never be taken longer than 12 years.
Chronic use of morphine = repetitive and pattern-followed morphine abuse that reflects negative consequences on:
- person’s economic stability
- social relationships
- state of health
Nervous System Effects
As opioid use in America rises, it becomes increasingly important that we better understand the neurological and behavioral effects of these drugs. There are some known risks of using morphine. In fact, doctors have come to expect drug dependence, cognitive impairment, and a phenomenon known as hyperalgesia, an increase sensation of pain triggered by the pain medication itself. Still, some nervous system effects are still be researched and discovered.
This 2011 article published in the medical journal, Pain, noted the specially noxious effects of morphine on the brain. Morphine was found to decrease the amount of gray matter in the amygdala, an area responsible for neural reward-processing. This 2015 article published in the medical journal, Neurologia, found that, “the actions of morphine on both developing and adult brains produce alterations in the plasticity of excitatory postsynaptic sites of the brain areas involved in limbic system functions of reward and learning.” What do these findings mean in layman’s terms?
These recent findings are important, because they point to physical changes that can reinforce drug addiction. In simple terms, the brain adapts to morphine by dulling our natural responses to food, sex, or pleasure…encouraging use to take morphine for rewards that we normally find naturally. Because morphine can not only change brain function but also changes the structures and form of the brain, we need to be thinking about how to better manage pain in the long term. More on this in the section about tapering below.
The main effects of morphine on the brain include:
- decrease in the volume of gray matter in the amygdala
- depressed consciousness
- diminished reflexes
- general psychomotor impairment
- possibility for seizures
- slowed reaction time


Neurotransmitters
Morphine is an incredibly potent analgesic pain reliever. Because it is known to cause strong addiction – and very uncomfortable withdrawal symptoms – doctors only prescribe morphine in cases of absolute need. In fact, the opiate has been found to affect over 10+ circuits in the brain. See the August, 2016 medical journal, Molecular Cells for a full list of brain reward circuits affected by morphine. Various changes are reflected in the distinct connectivity and function of brain reward circuits. Full article on Brain Reward Circuits in Morphine Addiction here.
Here are some of the ways that morphine affects neurotransmission.
- Morphine affects m-receptors, and also interacts at k- and d-receptors.
- It binds to opiate receptors within the limbic reward pathway.
- It binds to receptors concentrated in areas of the pain pathway.
- It causes sedation, relaxation and drowsiness
- Morphine gives short-term feelings of emotional well-being, warmth and pleasure.
- Morphine produces euphoria and elevated mood.
Here’s a graphic view of the neurological pathways that morphine affects:
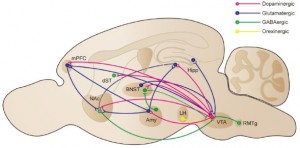

Personality and behavior
In addition to the serious risks of addiction, abuse, and overdose, the use of morphine can have a number of side effects to your mental health. It can trigger depression, mental clouding, or abnormal thoughts. Further, sleeping problems are common when taking morphine. Morphine use has also be connected with a feeling of disconnectedness. Long-term or high dose users have reported delirium.
All of these side effects can cause other changes to personality and behavior. Changes include:
- alterations in personality
- apathy
- destructiveness
- compulsion to use morphine
- inattentiveness
- lethargy
- neglecting formerly enjoyable activities and hobbies
- obsessive behavior over obtaining morphine
- sudden mood and action changes
What are typical morphine doses?
Only a doctor will be able to dose you appropriately with morphine. The risk for overdose and death is just too high to recommend dosing online. According to this FDA prescribing information for morphine sulfate oral solution, doctors are cautioned to be careful during dose selection, starting at the low end of the dosing range while carefully monitoring for side effects. Dosing errors with morphine are possible, due to confusion between different concentrations and between mg and mL. So, take care to ensure that you understand the proper dose is when beginning any morphine use.
Abuse typical doses
- Per day recreationally …… 30-60 mg orally as a starting dose
- Addicts can administer 1 to 3 times per day.
- Addicts with high tolerance to morphine can use 2000-3000 mg daily.
Lethal typical doses
- Overdose ………… 200mg is the least amount needed for overdose. But, in case of over sensitivity to morphine, 60mg can be fatal.
We understand it is difficult to talk to someone about your struggle. Check out our interactive Virtual Consultant to receive your treatment options easily.
Confidential and Free.
Occasional Tapering
When you’re taking morphine for long than a few weeks, a few things begin happening in the body. First, you develop drug dependence. This means that your brain and body adjust to the chemicals found in morphine in order to keep operating. In fact, they actually “speed up” some processes in order to counter the depressant effects of the painkiller. When you quit or lower dosage, you can expect specific symptoms of morphine withdrawal.
Second, you can expect to become more tolerant to morphine. Tolerance manifests as less effective pain relief, requiring more morphine more often in order to achieve therapeutic effect. Finally, morphine can produce hyperalgesia, a paradoxical increase in pain perception.
To counter these predicted effects, doctors suggest tapering anytime:
- Take dosages greater or equal to 50 morphine milligram equivalents a day
- You do not experience clinically meaningful improvement in pain and function.
- You experience overdose.
- You experience another serious adverse event.
- You shows signs of substance use disorder.
- You exhibit early warning signs for overdose risk such as confusion, sedation, or slurred speech.
You can find specific guidelines for tapering off morphine here:
CDC Guideline for Prescribing Opioids for Chronic Pain
Washington State Opioid Taper Plan Calculator
CDC Pocket Guide for Tapering Opioids









Related Posts